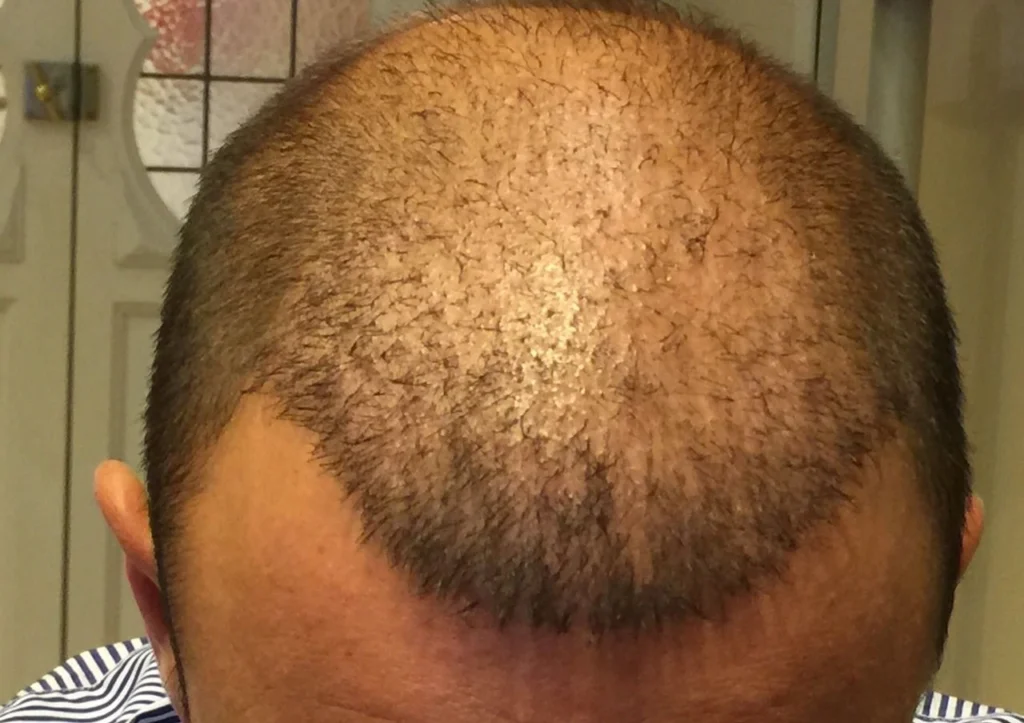
A proper evaluation looks at donor area quality, hair loss pattern, and overall health. This helps determine whether treatment is safe and what results are realistic. Solutions depend on the cause and may include waiting, using medical therapy, or planning corrective work.
In places like Hair Transplant Mexico in San Pedro, Monterrey, this process takes place in a structured hair transplant clinic with physician oversight and follow-up.
Key Takeaways
- A rejected hair transplant usually means the patient is not a good candidate due to limited donor supply, unstable hair loss, or health issues.
- Hair transplant failure is often linked to technical mistakes, poor graft handling, or weak postoperative care, not true rejection.
- A proper evaluation assesses the donor area, hair loss pattern, and medical history to guide safe treatment and avoid unsuccessful surgery.
- Signs of failure include low growth, patchy density, or an unnatural hairline, and these need medical review.
- Next steps may include delaying surgery, using medical treatments, or planning repair within donor limits.
Why You Were Rejected for a Hair Transplant
It is common for hair transplant patients to be told they are not good candidates. This step helps prevent failure and protects long-term results. Doctors who perform this procedure focus on safety and realistic outcomes.
Rejection is not always permanent. Some people can qualify later if their condition improves. This decision is often part of a long-term plan.
Donor Area Limitations
The donor area controls how many graft units are available. If there is not enough hair, it is hard to create good coverage. This is common in advanced hair loss.
Follicular Unit Extraction (FUE) needs healthy follicles. If the supply is low, transplanted grafts may not give enough density. This can lead to weak results.
Advanced or Unstable Hair Loss
Ongoing hair loss makes planning difficult. If natural follicles continue to thin, the final result may look uneven. This affects the overall result of the surgery.
Doctors may suggest waiting until hair loss slows down. Medical treatment can help stabilize the pattern. A stable donor gives better long-term results.
Medical Conditions and Risks
Some health conditions can affect healing and graft survival. Uncontrolled diabetes, scarring alopecia, and poor blood circulation can reduce blood supply to the scalp and limit growth.
Certain medications, such as blood thinners or immune-related treatments, can also affect recovery. A medical check helps identify these risks and ensure the procedure is safe.
Unrealistic Expectations
Some patients expect results that are not possible. This can lead to disappointment even if the surgery is done well. Expectations must match the available donor area.
A successful hair transplant depends on realistic goals. Doctors plan based on natural density and long-term results. This improves satisfaction.
How Hair Transplant Evaluation Works
Donor and Scalp Assessment
The first step is checking donor density and scalp health. This shows how many graft units can be used. Poor scalp health can reduce success.
This step helps prevent hair transplants from failing. It also helps plan natural coverage.
Hair Loss Pattern Review
Doctors study the hair loss pattern. They check if it is stable or still changing. This helps predict future results.
If the pattern is unstable, gaps may appear later. Planning accounts for this risk.
Medical History and Planning
Doctors review your health history and treatments. This helps find risks that may affect healing. It also guides safe planning.
The plan sets clear and realistic goals. This helps avoid an unsuccessful transplant.
Hair Transplant Failure: Causes and Risk Factors
Hair Transplant Failure Rate
Failure rates are usually low in properly selected cases. In general, an unsuccessful transplant may occur in about 5% to 15% of cases, depending on factors such as patient selection, surgical technique, and postoperative care. The risk is higher when procedures are performed without proper planning or by inexperienced surgeons.
Understanding this range helps set realistic expectations. It also highlights why a thorough evaluation and proper technique are important to reduce the risk of failure.
Surgical and Technical Factors
The skill of the hair transplant surgeon is important. Inexperienced surgeons may damage follicles or place grafts poorly. This can affect growth and appearance.
Grafts must be handled with care. If they stay outside the body too long, survival drops. This increases the chance that hair transplants fail.
Post-Procedure Care Issues
Postoperative care is critical for graft survival, especially in the first 7 to 10 days. For a full breakdown of recovery steps, see this guide on post-hair transplant care.
Touching, scratching, or applying pressure to the scalp can dislodge transplanted grafts before they anchor. Washing too aggressively or too early can also affect healing and reduce growth. During this phase, it is also important to understand how hair transplant scabs form and heal.

Other factors, such as smoking, alcohol after a hair transplant, and sun exposure, can slow recovery and affect blood flow to the scalp. Not following cleaning routines or skipping follow-up visits can increase the risk of follicle transplant failure. Careful adherence to instructions helps protect each graft and supports stable results.
6 Reasons Hair Transplants Fail
1. Poor Candidate Selection
Not every patient is a good candidate for surgery. Low donor density, advanced hair loss, or unstable patterns can limit results. When a procedure is performed on a poor candidate, the available graft supply may not provide adequate coverage. This often leads to an unsuccessful transplant, even if the technique was correct.
2. Improper Surgical Technique
Technical errors during the procedure can damage follicles. This includes poor graft handling, incorrect placement angles, or excessive time outside the body. These mistakes reduce graft survival and affect the final result. Even small errors during implantation can lead to uneven growth or unnatural appearance.
3. Low-Quality or Limited Donor Hair
The quality of the donor area directly affects outcomes. Weak or thinning follicles may not grow well after transplantation. In some cases, there are simply not enough grafts to achieve the desired density. This limits what can be achieved and increases the risk of failure.
4. Inexperienced Surgeons or Clinic Setup
Experience plays a major role in results. Inexperienced surgeons may damage follicles, misplace grafts, or design unnatural hairlines. Some clinics rely on high-volume models with limited medical supervision. This increases the risk of inconsistent outcomes and poor planning.
5. Poor Post-Operative Care
Postoperative care is essential for graft survival. Touching the scalp, exposing it to the sun, or failing to follow instructions can dislodge transplanted grafts. Smoking, alcohol, or poor hygiene can also affect healing. Even a well-performed procedure can fail if recovery is not managed correctly.
6. Underlying Medical or Scalp Conditions
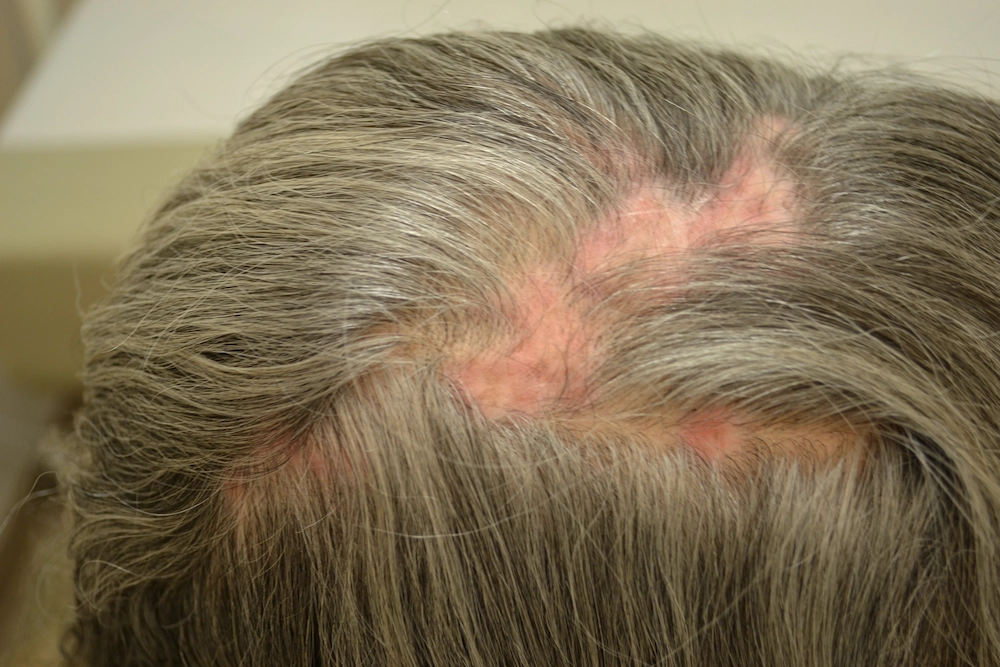
Certain conditions can affect healing and follicle survival. These include autoimmune disorders, scarring alopecia, or chronic diseases that reduce blood flow. Inflammation or poor scalp health can prevent transplanted grafts from growing. In rare cases, this may resemble graft rejection, although true biological rejection is uncommon.
Signs and Appearance of a Failed Hair Transplant
There are several visible signs that may indicate an unsuccessful procedure. These signs help patients understand whether the result is progressing normally or requires evaluation. While some changes can be part of the healing process, others may point to issues with graft survival or design.
- Low Growth or Graft Survival: Low growth is a key sign of failure. Hair may grow slowly or not at all if grafts were damaged. A proper check helps identify the cause and guide next steps.
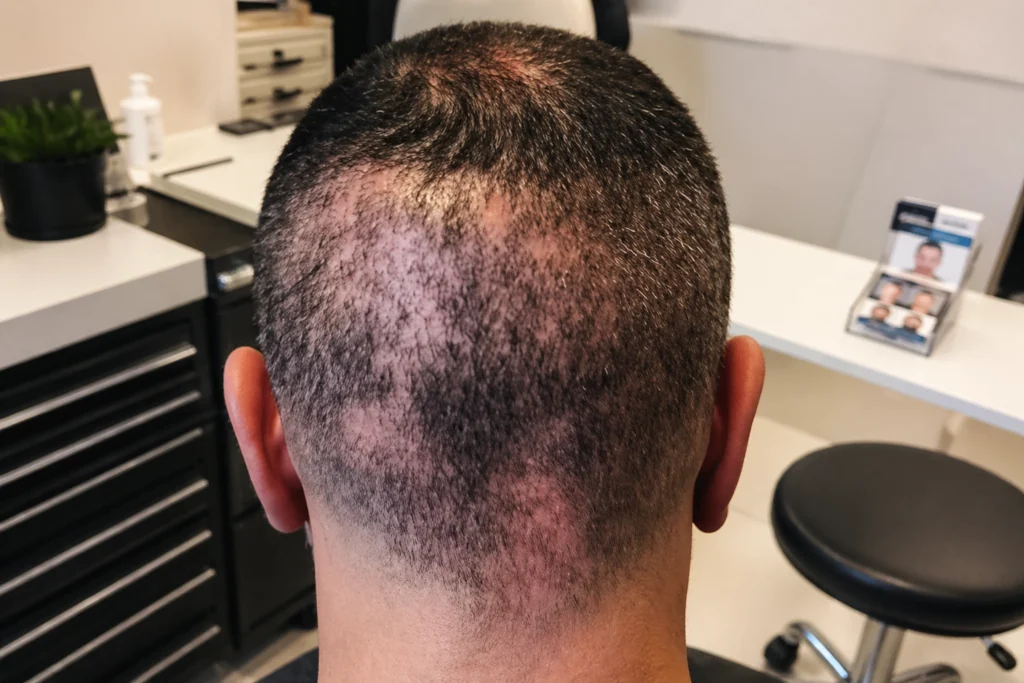
- Uneven Density or Patchiness: Patchy areas show uneven growth, with some spots appearing full and others thin. This affects the overall look and may result from poor placement or low graft survival.
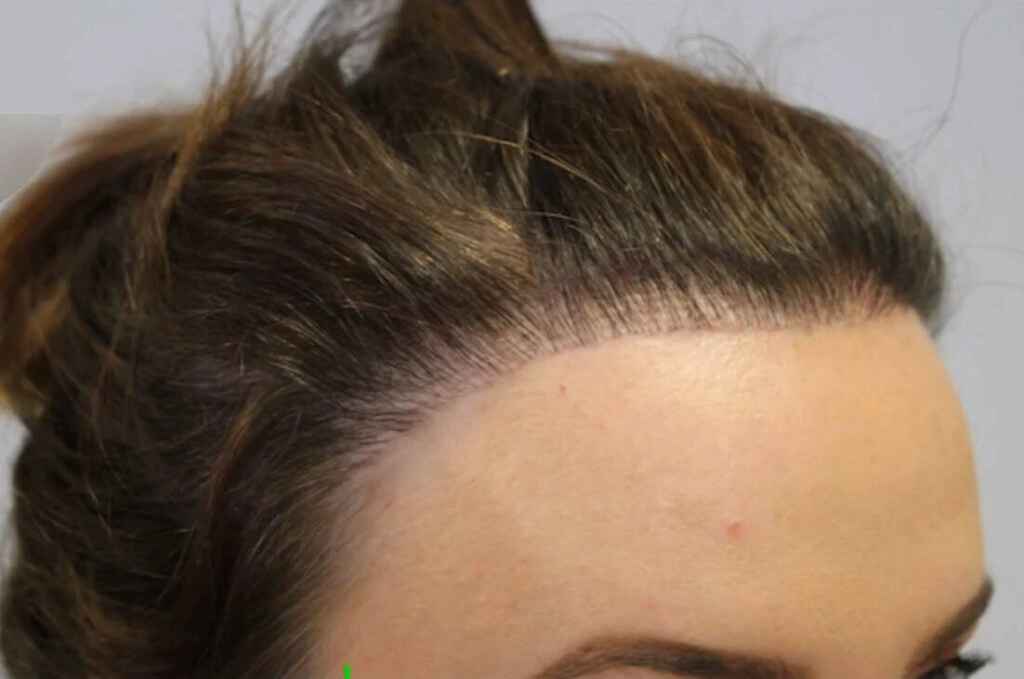
- Unnatural Hairline Design: A poorly designed hairline may look too straight or too dense, making it noticeable. Natural results require careful planning and balanced placement.
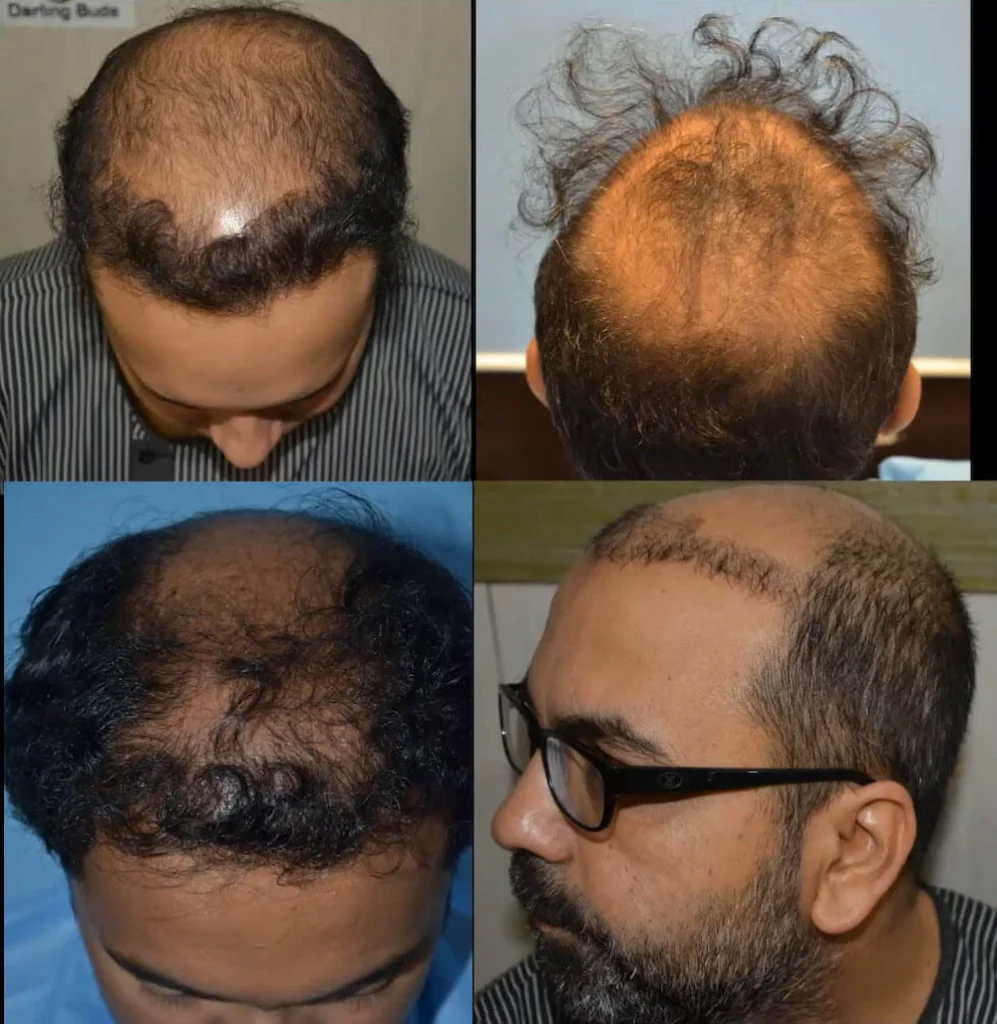
- Failed Hair Transplant Photos Explained: Photos may show low density or poor shape, but they can be misleading. The lighting and healing stage affects appearance, so focus on spacing, visible scalp, and direction issues, and confirm with a medical evaluation.
Hair Transplant Failure After 2 Years
Ongoing Hair Loss Progression
Hair may keep thinning after surgery. Transplanted grafts may remain, but natural follicles can fall out. This changes the look over time.
Planning must include future hair loss. Follow-up helps adjust treatment. Long-term expectations can be better understood by reviewing results from a hair transplant after 10 years.
Late Shedding vs Permanent Loss
Late shedding can be normal. Permanent loss may mean graft failure. A doctor can tell the difference.
Understanding timing helps avoid wrong conclusions.
Hair Transplant Timeline and Expected Results
Hair growth takes time. Early changes are normal and not always a failure.
- 0 – 3 months: shedding phase
- 4 – 6 months: early growth
- 9 – 12 months: visible change
- 12+ months: stable result
Patients should also understand when it is safe to trim their hair by reviewing guidance on haircuts after a follicle restoration surgery.
Repair Options After Hair Transplant Failure
Repair depends on the cause and donor limits. In some cases, additional graft units can improve density. If the issue is design, the hairline may be adjusted for a more natural look.
Common options include:
- Secondary transplant to add density
- Hairline correction
- Scalp micropigmentation
Planning depends on the availability of donor grafts and realistic expectations.
Donor Area Management Limits
The donor area must be protected. Overuse reduces future options. This limits repair work.
Careful planning avoids more damage. The goal is safe improvement.
What to Do Next Based on Your Situation
Next steps depend on your case, but each situation has a clear path. If you were rejected, the focus should be on improving your candidacy before considering surgery again. This may include stabilizing hair loss with medical treatment and reassessing the donor area after a few months.
If you had an unsuccessful transplant, the first step is to identify the cause. A physician should evaluate graft survival, hairline design, and donor condition before planning any correction. In many cases, waiting 9 to 12 months for full results is necessary before deciding on repair.
What to Do if You Are Not a Candidate
Medical Treatment Options
Medical treatments can help slow hair loss and improve scalp health. These are often used when a patient is not ready for surgery or is a poor candidate.
Common options include:
- Minoxidil to stimulate hair growth
- Finasteride to reduce hair loss progression
- Anti-inflammatory treatments for scalp conditions

A doctor will choose the right option based on the patient’s condition and long-term plan.
Non-Surgical Solutions
Non-surgical methods can improve appearance without surgery. Some patients explore alternatives to hair restoration surgery when surgery is not the right option. These options are useful for patients who are not candidates for a procedure or who prefer to avoid one.
Common options include:
- Scalp micropigmentation to reduce the look of thinning
- Hair fibers or concealers to add temporary density
- Hair systems or wigs for full coverage
These methods do not replace follicle restoration surgery, but they can improve visual results.
Re-Evaluation Over Time
Your status can change. You may qualify later if conditions improve. Regular follow-up helps reassess. This supports safe planning.
Safety and Risk Considerations
Importance of Physician Oversight
Doctor involvement improves safety. A trained specialist plans and performs the procedure. Some clinics have less supervision. This can affect the results in any hair transplant clinic.
Surgical Risks and Complications
All procedures have risks. These include infection, poor healing, or graft loss. Clear communication helps patients understand risks. This supports safe decisions.
Setting Realistic Expectations
Expectations affect satisfaction. Results depend on donor availability and scalp condition. Clear goals reduce disappointment. This leads to better outcomes.
Clinical Factors That Influence Outcomes
Many factors affect results. These include blood flow, healing, and overall health. Handling of transplanted grafts is also important. These factors explain different outcomes. A full evaluation looks at all these elements. This helps improve consistency and safety.
If you are unsure about your candidacy or results, a proper medical evaluation can provide clarity. Scheduling a consultation allows a qualified physician to review your case and outline safe, realistic next steps based on your condition.